


Chemicals start flooding the brain, and in an instant, a rush of enjoyment follows.
What caused the reaction could be any number of things: a forkful of chocolate cake, a kiss from the person you love or the opening notes of your favorite song.
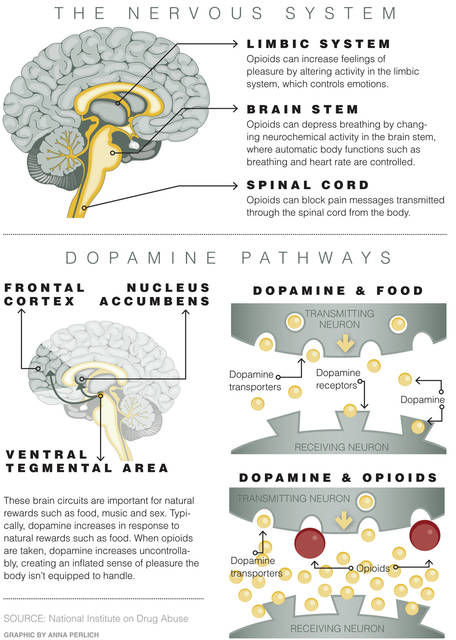
Dopamine, one of the brain’s chemical messengers, is involved in dozens of vital functions including breathing and walking. The hormone also rewards behavior with an enjoyable feeling.
Normally, the brain has a system in place to check how much dopamine is released and at what speed. When someone takes opioids, which are prescription pain killers or heroin, the guards are gone. The hormone is allowed to flood the body uncontrolled, like a car gaining speed as it travels down a hill.
“All of the sudden, the brain sees the receptor gone away. There are no brakes anymore, it only accelerates,” said Dr. Ruben Baler, a neuroscientist and health science administrator for the National Institute on Drug Abuse.
Dopamine and its impact on the body is the key to understanding the runaway effect opioids have on the body. Each dose of the drug causes a biological reaction. Pathways in the brain are altered, which drives behavior and continued use of the substance.
Powerful opioids such as heroin, fentanyl and oxycodone re-circuit the brain so quickly that a person becomes dependent. For doctors and researchers studying the ongoing opioid epidemic, it is clear that addiction to these drugs is driven by biology, not a moral or personal failing.
“The parts of the brain that help us consider cause and effect come offline in addiction,” said Dr. Joseph Niezer, a psychiatrist with Franciscan Health Network Psychiatric Specialists in Indianapolis. “There are identifiable changes in the brain of someone dealing with addiction, the same way there are changes with someone who had Parkinson’s disease or Alzheimer’s disease.”
It’s an illness
Addiction is officially recognized as a brain disease, a chronic, relapsing condition in which a person compulsively seeks out and uses drugs despite continued harmful consequences, according to the American Society of Addiction Medicine.
Estimates from the National Institute on Drug Abuse report that 2.6 million people suffer from substance use disorders related to prescription opioid pain medications and heroin.
But many more people take medication as prescribed and have no problems stopping using, or even in some cases do misuse or abuse those drugs, and do not become addicted. But some people are at a genetic disadvantage to become dependent on these drugs, Baler said.
“Just talking about one gene, and there are thousands of genes that we can talk about that can impact it,” Baler said. “Individually, these gene differences are not huge. But if you add them up, you are building up personalities that are more likely to engage in drug abuse, and once they’re exposed to that, they’re more likely to repeat the experience over and over again.”
Environment can also impact who falls into addiction. People who suffer from chronic sleep deprivation have a lowered ability to regulate dopamine.
People who have dealt with chronic pain and have taken legal, prescribed opioid medications can find their bodies becoming more and more tolerant to the substances. The same dosage that used to relieve their pain no longer does, and side effects such as nausea and vomiting are lessened. As the impact the drugs have on the brain decreases, higher doses are required, which can also eventually lead to dependence, Baler said.
“All of these things — genetic and environment — react in very complex ways. The result is this huge range of individual differences in the people who, once exposed to those drugs, who want to repeat this experience and risk becoming addicted to it,” Baler said.
‘Once I got a taste for it, I was gone’
Shayna Wheeler realizes now that she had the unlucky combination of genetic, environmental and social factors that dragged her into addiction.
For 16 years, the Indiana resident was addicted to substances of all kinds, starting with alcohol and pain medication, then moving on to crack cocaine, meth and heroin.
As a teenager, she started drinking beer and smoking pot, like most of her classmates and friends. She doesn’t know why they were able to use drugs recreationally and stop when they needed to. Though starting to drink and smoke pot was her choice, getting high became a compulsion.
“I was out of the gate as an addict,” she said. “I was always a smart girl, a cheerleader, on the honor roll. But once I got a taste for it, I was gone.”
The impact that opioids have on the brain stems from the way humans have evolved, Baler said.
The brain has evolved over millions of years to help drive and encourage survival of our species. For example, eating, reproducing and taking care of the young can all provoke the release of chemicals, particularly dopamine, to make a person feel good.
If you feel enjoyment after eating or having sex, you’re going to keep doing it, which allows humans to persist as a species, Baler said.
“There is a very primitive, very robust system that rewards behaviors that we want to be repeated, because natural response reinforces that for survival,” he said.
Evolution has provided a mechanism for humanity to survive over tens of thousands of years, but it does not occur quickly, Baler said. Elements of the environment we live in — the activities we take part in, the entertainment we watch and the substances we consume — are rapidly changing.
That environment can provide rewards to the nervous system much greater than what the brain was designed to handle.
Baler compared the natural release of dopamine for different activities on a one to 10 scale. Eating a delicious meal or having a fun night out with friends will raise dopamine levels somewhere in that natural range.
The brain operates on a kind of biological thermostat, adjusting how the hormone is released and never letting that level get too high, Baler said.
Different drugs can throw the entire system in chaos.
“Things such as amphetamine and opioids can trigger that dopamine well beyond anything evolution has ever intended, to a magnitude of 100 or 1,000,” Baler said. “The thermostat now is at risk, because it hasn’t been designed to deal with these values of dopamine.”
Opioids in particular short-circuit that system, blocking a chemical called a receptor that would check dopamine production. The drugs take away the natural abilities of the brain to curtail the release of dopamine. When someone takes heroin, morphine or another drug of this type, dopamine production runs uncontrollably.
Such high levels of dopamine in the brain warp the natural tolerance for the chemical, and the biological urge is to replicate that feeling. The only way to do so is with an opioid such as vicodin or oxycodone, powerful painkillers available by prescription only. Heroin, a highly addictive street drug derived from morphine, also achieves the same effect, but is much cheaper to buy.
The ability of those drugs to spike dopamine to abnormally high levels is what leads to addiction, Baler said.
‘You have to have it’
What makes addiction a disease is that as drugs are used over and over, the substances can change the structure of the brain and how it works.
Opioids such as heroin, fentanyl and carfentanil are so powerful that addiction can form more quickly and in smaller doses, said Kim Manlove, retired director of the Indiana Addictions Issues Coalition.
“The more you use it, it causes more intense feelings of pleasure,” he said. “It gets to the point where you just want to use it over and over again.”
The drugs also shape the brain’s memory center, inhibitions and motivational systems, essentially hijacking the entire function of the brain to focus on the next hit.
In particular, the motivation center of the brain is impacted. That primitive area of the brain is rewired so that the drug is as important as food, water, breathing and other life functions. That’s why people keep using it, despite the consequences. They can rationalize their drug use, Niezer said.
“Addiction is really the using despite the negative consequences. There are plenty of people who take opioids and are not overusing them or continuing to use them despite the consequences,” Niezer said. “With people who are addicted, even though this drug is causing all the problems in this person’s life, there’s this thought that if they use, everything will be OK.”
The way that opioids change the brain doesn’t just make addiction possible; it also makes quitting, and relapsing once you try to quit, much more likely.
Addiction is a chronic disease, because it can impact people for their entire lives, Manlove said.
“Your brain actually craves it and wants it, and overrides the other parts of the brain that says you really shouldn’t do it,” he said. “You need to have it, you have to have it.”
Recovery doesn’t move in a straight line, Wheeler said. You don’t decide to be clean and then it’s all upward trajectory; there will be stumbles, and between 40 and 60 percent of people who receive treatment for drug addiction will suffer relapse, according to the National Institute on Drug Abuse.
“You can’t necessarily put a success rate on addiction. You can’t measure one person’s success on getting past addiction on another person,” she said. “Relapse is a part of recovery.”
Breaking through those intense cravings, and helping people repair their changed brains so that they don’t need to go back to the drugs, requires extensive long-term treatment, including medications, counseling and support.
Part of the reason that U.S. is seeing such a crisis with opioids is that historically, the treatment model has focused on short-term inpatient care, rather than treating a chronic disease, Manlove said.
They go to detox, they quit the drug and they receive some short education about addiction. Then, they are referred to 12-step programs or other groups that, while effective for some, don’t provide the same level of care, including medication, that is needed to overcome the disease.
“We don’t do that with other chronic medical diseases like diabetes and cancer. If you’re diagnosed with cancer, you get radiation and drugs and five years of annual checkups and continuing care,” Manlove said. “But historically, (addiction) has been a shame-based disease, that it’s a personal choice and they’re doing this because they want to.”





