SIDNEY — The American Heart Association (AHA) has reported almost 30 million Americans have coronary heart disease. It is the leading cause of death in the United States.
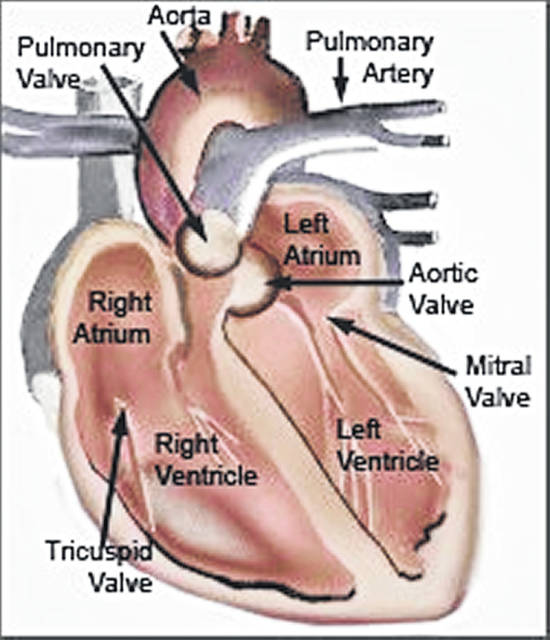
Coronary heart disease or CHD (also called coronary artery disease or CAD) occurs when the arteries that supply blood to the heart muscle become hardened and narrowed. This can affect even the smallest arteries that feed the heart. The main artery from the heart is the aorta. Veins carry oxygen-poor blood back to your heart. At the lungs, it is the pulmonary artery that brings oxygen-poor blood into the lungs and the pulmonary vein that carries oxygen-rich blood back to the heart. According to the National Heart, Lung, and Blood Institute (NHLBI) coronary heart disease is the number one killer of both men and women in the U.S., with nearly half a million Americans dying of heart attacks and/or cardiac arrest caused by CHD each year.
“Many of these deaths could be prevented because coronary heart disease can be related to certain aspects of lifestyle,” said Dr. Ryan Clark, cardiologist at Wilson Health. “Among the lifestyle risk factors that can be controlled are: smoking, obesity, physical inactivity and drug abuse. High blood pressure and high blood cholesterol also increase the risk of developing CHD. In addition, certain things beyond our control, such as family history and age, increase risk as well.”
How heart disease develops
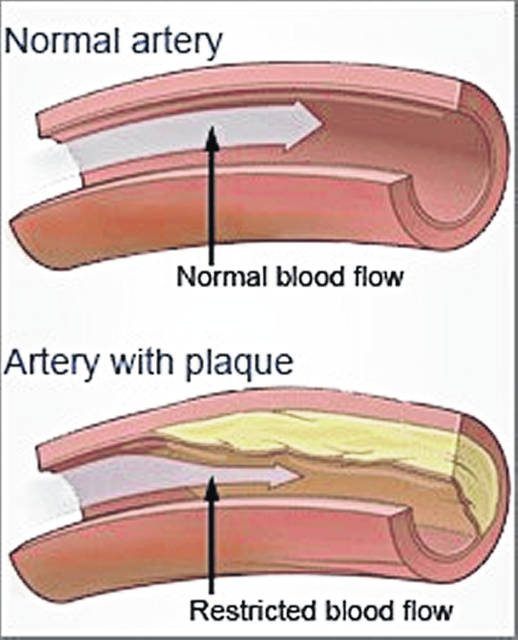
“Basically, your heart is a muscle,” said Clark. “In order for it to function, it needs a good supply of oxygen and nutrients. But sometimes, the coronary arteries become narrowed or clogged and cannot supply enough blood to the heart. This results in what’s called atherosclerosis.”
Atherosclerosis usually occurs when a person has high levels of cholesterol, a fat-like substance, in the blood. Cholesterol and fat build up on the walls of the arteries. The build-up of cholesterol, fat and other substances is called plaque. This process begins in most people during childhood and the teenage years, and worsens as they get older.
“Because symptoms and severity can vary so much from person to person, there is no one single test used to diagnose CHD,” said Clark.
Among the diagnostic tools that can be used are:
• Electrocardiogram (ECG or EKG), which is a graphic record of the electrical activity of the heart as it contracts and rests
• Stress test or treadmill test, which is used to record the heartbeat during exercise
• Cardiac catheterization, coronary angiography or arteriography, which are tests used to explore the coronary arteries, using a fine tube (catheter) that’s put into an artery of an arm or leg and passed through the tube into the arteries of the heart
• Echocardiography, which uses sound waves to create an image of the heart
• CT Scan, which is an imaging technique that provides cross-sectional images of the chest, including the heart and major vessels
• Magnetic Resonance Imaging (MRI), which uses powerful magnets to produce computer-generated pictures of the heart and major vessels
• Nuclear scanning, which is sometimes used to show damaged areas of the heart and expose problems with the heart’s pumping action
The choice of diagnostic tool depends on a variety of factors including a patient’s medical history and individual health problems.
Treatment options
Many things are considered when choosing treatment options for someone with coronary artery disease. Factors to be considered include the extent of the disease, the symptoms, the person’s overall health and whether there are other medical conditions such as kidney disease, diabetes or previous heart attack or stroke.
“For many people, CHD can be managed with lifestyle changes and medications, although some people also require surgery,” says Dr. Clark.
Lifestyle – Specific recommendations should always be discussed with a doctor, but there are changes many people with CHD can make to improve their health. Some suggestions from the American Academy of Family Physicians are:
• Stop smoking
• Switch to a low fat diet
• Avoid saturated fats
• Maintain desirable cholesterol and blood pressure levels
• Lose weight if needed
• Exercise
Medication: These include “beta-blocker” drugs that decrease the workload on the heart and can reduce the risk of heart attack; nitroglycerine and other “nitrates;” and “calcium-channel blockers” that relax the arteries. The tendency to form clots may also be reduced by aspirin or by other platelet inhibitory and anticoagulant drugs. For those with elevated blood cholesterol, cholesterol-lowering drugs may be prescribed. Impaired pumping function of the heart may be treated with digitalis drugs or ACE inhibitors. And if there is high blood pressure or fluid retention, these conditions are also treated. If medications are prescribed, always ask your doctor what the medication is, what it does, and whether there are any side effects.
If lifestyle changes and medications aren’t enough, surgical options may be needed.
Angioplasty: One option is coronary angioplasty or balloon angioplasty. In this procedure, a fine tube, or catheter, is threaded through an artery into the narrowed heart vessel. The catheter has a tiny balloon or other device at its tip, that is used to open or stretch the artery. This is done to improve blood flow, after which the tube is removed.
Stents: Stents are often inserted during angioplasty to help keep the artery open. A stent may also be used without angioplasty. Basically, a stent is a wire mesh tube that’s inserted into an artery to help keep it from closing up again. Even with a stent, however, an artery can reclose, requiring either another angioplasty or a bypass. NHLBI says this is especially common for people with diabetes or unstable angina.The new re-narrowing is called in-stent restenosis. AHA says the use of stents, coated with drugs to help keep the vessel from closing, can help to reduce this risk. Brachytherapy can also be used, according to the Food and Drug Administration (FDA). It is a procedure in which radioactive material is placed into the body. After initial opening of the in-stent restenosis blockage with a balloon catheter (PTCA), a brachytherapy device is temporarily placed at the site of the in-stent restenosis. FDA says the radiation treatment prevents an exaggerated healing response at the lesion site and a recurrence of a significant blockage.
Bypass: Another surgical option is a coronary artery bypass operation. In this procedure, a blood vessel, usually taken from the leg or chest, is grafted onto the blocked artery, bypassing the blocked area. If more than one artery is blocked, a bypass can be done on each. The blood can then go around the obstruction to supply the heart with enough blood to relieve chest pain. In many cases, besides fixing the artery that is blocked, the surgeon will fix additional arteries on the heart that are starting to look blocked. The number of arteries repaired becomes the name of the procedure. For example, if the surgeon repairs three of the arteries, it is called a triple bypass. If four arteries are repaired, it’s a quadruple bypass. Sometimes, more than one bypass operation is needed. A bypass also can close again. NHLBI says this happens in more than 10 percent of bypass surgeries, usually after 10 or more years. The important thing to remember is that coronary heart disease is a serious diagnosis, and it requires a lifetime of vigilance in order to stay healthy. Although medication and surgery may relieve the symptoms of heart disease, you also need to make the changes necessary to develop a healthy lifestyle as well.
“The important thing to remember is that coronary heart disease is a serious diagnosis, and it requires a lifetime of vigilance in order to stay healthy,” said Clark. “Although medication and surgery may relieve the symptoms of heart disease, you also need to make the changes necessary to develop a healthy lifestyle as well.”



